
Home
Voor patiënten en familieleden
Voor medische specialisten
Onderzoeksteam
Actualiteiten
Home For patients and families For medical specialists Research team Current events
FOR PATIENTS AND FAMILIES
Nephronophthisis
Nephronophthisis is one of the most common genetic causes of kidney failure in children. In the most prevalent form of this disease, the juvenile form, kidney failure develops at an average age of 13 years. Because the symptoms can be aspecific or difficult to detect, it can take long before nephronophthisis is diagnosed. Symptoms can be: excessive drinking and passage of urine, growth delay and chronic anemia. If these symptoms are present, the pediatrician or pediatric nephrologist will investigate the kidneys and the kidney function. Nephronophthisis causes a reduction of kidney function due to scarring (i.e. ‘fibrosis’) of kidney tissue. In some cases, an ultrasound will reveal kidney cysts. In addition, nephronophthisis can occur in combination with symptoms of other organs.
Hereditary factors in nephronophthisis
There are several genetic factors (or ‘genes’) known in which alterations can cause nephronophthisis. The genes that have been discovered so far encode proteins that have a function in the cilia. Cilia are ‘hair-like’ structures that are present on the surface of kidney cells. They are involved in the detection and the transmission of signals from and towards the cell. The function of the cilia is disrupted in nephronophthisis. As a result, nephronophthisis belongs to the group of ‘ciliopathies’, or conditions that involve the cilia.
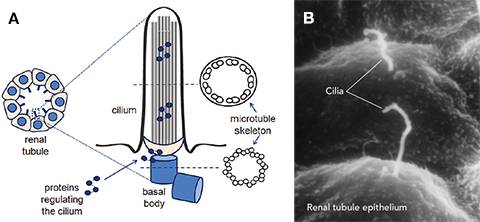
Figuur 1. Cilia.
A. Schematic representation of a cilium. Proteins move along the skeleton of microtuli from the base of the cilium (the ‘basal body’) to the tip of the cilium and back.B. Cilia on the surface of kidney cells seen through an electron microscope. Source: Zhang Q, Taulman PD, Yoder BK. Cystic kidney diseases: All roads lead to the cilium. Physiology. Aug 2004; 19(4):225-30.
In the majority of patients with nephronophthisis, the underlying genetic defect is unknown. This means that we have not detected an alteration in the currently known nephronophthisis genes. We use DNA testing to discover new genes that are involved in the development of nephronophthisis.
Other Symptoms
Next to kidney cells, cilia are present on other cell types, for example cells in the eyes, the liver, the brain and the bones. As a result, nephronophthisis can occur in combination with other symptoms like blindness or intellectual disability. In these cases, nephronophthisis is part of a syndrome. A syndrome is a combination of symptoms with one underlying cause. Examples of syndromes associated with nephronophthisis are Joubert syndrome, Bardet-Biedl syndrome, Jeune syndrome and Sensenbrenner syndrome.
> read more about these and other syndromes on Genetics Home Reference
What do we investigate
The goal of the KOUNCIL study is to improve diagnostics and treatment of nephronophthisis and nephronophthisis-related syndromes. The different components are explained below.
DNA testing
To improve our understanding of the genetic background of nephronophthisis, we use a new technique called ‘whole-exome sequencing’. ‘Whole-exome sequencing’ is an extensive DNA test used to analyze all of the protein-coding parts of the DNA. This means that we can analyze all of the known nephronophthisis genes simultaneously and discover new genes.
Investigation of urine
Kidney cells are excreted in urine. A new technique enables the isolation of kidney cells from urine to investigate the effect of a variant in the DNA. For example, we can investigate whether a genetic variant leads to alterations in protein production or cilia function. Investigation of urine-derived kidney cells is only possible when patients have not had a kidney transplantation.
Database
We collect the results from DNA testing and medical information of nephronophthisis patients in an international nephronophthisis database. We will use the database to investigate the correlation between a variant in the DNA and symptoms in patients. In addition, we use the database to identify early symptoms of nephronophthisis. We aim to improve early diagnostics of nephronophthisis and genetic counseling for nephronophthisis patients. All medical information in the database will be coded to guarantee the privacy of participants.
Investigating disease mechanisms
We aim to unravel the disease mechanisms underlying nephronophthisis using molecular studies. In cells derived from a patient, we analyze the cilia and compare its morphology and function to the cilia of healthy individuals. In addition, we study the interaction network of nephronophthisis proteins, which cause the disease when they are not functioning properly.
Investigating new therapies
There is currently no treatment that prevents the decline in kidney function in children with nephronophthisis. Investigation of the genetic factions that can play a role in the development of nephronophthisis can lead to the identification of potential new targets for the treatment of nephronophthisis. Potential new drugs are first tested in zebrafish. Zebrafish are a suitable animal model to investigate nephronophthisis. Finding a drug that ameliorates the symptoms of nephronophthisis in zebrafish is a first step towards discovering a drug that can treat nephronophthisis in humans.
How to participate
Both patients with suspected nephronophthisis in whom the diagnosis has not been confirmed with DNA testing and patients with a confirmed diagnosis can participate in the KOUNCIL study. If the diagnosis has not been confirmed with DNA testing, we ask participants (and their parents if possible) for a blood sample to perform DNA testing. We ask patients who have not had a renal transplantation for a urine sample. We ask all participants consent to include their medical information in the database and to publish anonymized results from this research in medical literature.
More information
For more information on how to participate, see contact.
© 2015 www.kouncil.nl



